August 2018 Newsletter
In the Media

Dr. Melina Roberts has a published article in Amber Approved Magazine Summer Edition 2018 on 6 Factors that Contribute to a Fungal Infection.

Dr. Melina Roberts was a guest on Doctors Health Press podcast Episode 010: Treating Cancer From A Biological Medicine Perspective – Speaking with Dr. Melina Roberts, ND

Dr. Melina Roberts is honoured to be selected by her mentor and creator of Biological Medicine, Dr. Thomas Rau to be a lecturer for Swiss Biomedicine Academy – North America.
Upcoming Event
FREE Webinar: Lyme Disease & Chronic Infections: When Antibiotics Fail
Most patients do not experience complete resolution with antibiotics. We’ll explore the issues preventing people from recovering from these infections. These obstacles include: mold exposure, dental infections, SIBO, SIFO, parasites, trace mineral depletion, lymphatic congestion, adrenal issues, etc. We’ll also discuss the assessments that can be done to identify these obstacles.
Presented by Dr. Shaun Riddle
Date: Wednesday, August 22 at 7:30 PM – 9 PM EDT
Featured Article
The Common Dandelion: Rethinking a Misunderstood and Undervalued Weed
BY: DR. JATISH KALER

As a gardener I have tended to view the dandelion as an unwanted intruder, as it invades every nook and cranny of free space on a cherished lawn or garden. I think of sore backs and sorer knees from the countless hours spent uprooting these pervasive pests. And yet there is a softer side to the dandelion; the sweet memories of childhood wistfully blowing dandelion fluff to count our number of admirers and the dandelion stem bracelet used to seal a blossoming friendship or budding romance. Most remarkably, this common weed has a long and storied history in traditional medicines across the globe, with its oldest record of use dating back to Arabian physicians of the 10th and 11th centuries.
The scientific name for the dandelion is Taraxacum officinale, derived from the Greek words “taraxis” for inflammation and “akeomai” for cure. It is then no surprise generations have employed the dandelion to relieve the inflammation of hepatitis, gastritis, bronchitis and arthritis. In fact, modern research has proven many of the nutrients and phytochemicals in the dandelion to lower rates of inflammation and chronic disease.
Featured NEW Therapy
10-Pass Ozone Therapy
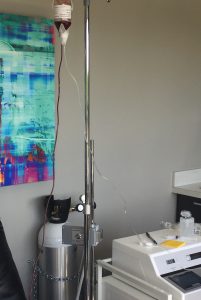
Intravenous ozone is an oxidative therapy where blood is drawn from a vein, ozonated and then re-infused back into a patient. It significantly increases oxygen utilization in the body. This means that it increases mitochondrial output of energy. That energy it produces is then used by the body immune and repair systems. This process could be thought of as “1-pass” of ozone.
Recent advancements in technology from Germany have enabled a patient to receive 10 passes of ozone in the same amount of time as the typical single pass treatment. This significantly increases the efficacy of the treatment.
The 10-pass is a very powerful and safe treatment. It is used to treat infections, inflammation, auto-immune disease, chronic fatigue and fibromyalgia, chronic pain, and multiple neurologic conditions including Parkinson’s, multiple sclerosis, stroke, brain and spinal cord inflammation of various types. It can treat Lyme disease, shingles, recurrent herpes simplex, influenza and pneumonia.
10 Pass Ozone Therapy, The Greatest Disease Fighting Tool
Featured Lyme Disease Blog
The Perils & Pitfalls of Lyme Testing
BY: DR. SHAUN RIDDLE

Like all other aspects of this illness, the topic of testing is complicated too. I’m going to try & unpack it here in a way that makes sense.
There are basically 2 ways to test for Lyme disease & its co-infections….
- Specifically test for the presence of the bug in the blood
- Test for immune system markers that indicate the body has seen the bug
Obviously, a positive test for the bug itself would be the best & most direct method for diagnosing Lyme disease. These tests are known as PCR (polymerase chain reaction) tests. PCR blood tests identify the DNA of a bug in the blood stream.
However, Borrelia doesn’t like to live in the blood stream. So relying on a blood test to find the actual bug doesn’t make much sense. Borrelia prefers to live inside cells & tissues so when a PCR blood test comes back positive for the Lyme, I consider it lucky. But a negative PCR test for Lyme does NOT means a person is negative.
There is a newer test available which tests for the presence of Borrelia in the urine. It is also a PCR test looking for the bug’s DNA but in this case, in a patient’s urine. Since urine is essentially filtered blood, this test also has the same issues. So the idea behind this test is to coax or “provoke” the bug out of hiding and into the blood stream prior to collecting urine.
There are several methods of doing this including: vigorous exercise, Rolfing or another deep tissue massage, & more recently, using ultrasound over specific areas of the body prior to the urine collection to drive some of the bugs temporarily into the blood stream. This may become the preferred method of testing once the ideal method of provocation has been worked out.
By far, the most common way of testing for the bugs is looking for antibodies to the infections in the blood. Antibodies are proteins our body makes in response to invaders. Antibodies bind to infections in an effort to destroy and facilitate their elimination. Vaccines work by stimulating the body to produce antibodies to infections before our body comes into contact with the bug. So if tested, most people would have antibodies in their blood to the measles virus for instance, even though they never got measles.
If you test positive for Lyme antibodies, it means your body has seen the bug. Conventional medicine will often argue that the presence of antibodies does not mean that you have a current infection. They argue that you had an infection in the past and your body cleared it. The problem with that explanation is that Lyme disease & its co-infections are bugs that are designed to live in our bodies long-term. In my experience, people rarely clear these bugs on their own.
There are several issues with testing for antibodies to Lyme & its co-infections. The test is really a test of a person’s immune system. However, Bartonella is a known immune suppressant. So if there is a co-infection of Bartonella present, a person is less likely to test positive for Lyme antibodies, for instance.
Another issue that was mentioned earlier is that Lyme disease doesn’t like to live in the blood stream. It prefers living inside cells & deeper tissues. Antibodies can drop over time when the bug is not “seen” by the immune system for a while.
The Lyme bug is also known to shift the markers it carries on the outside of itself in an effort to avoid detection by the immune system. These markers are the binding sites for antibodies. The immune system is making antibodies that are specific to these markers. If the markers are constantly changing, antibody levels can go up & down pretty quickly creating confusion on a test.
Without a specific marker that was present earlier to continue to trigger antibody production, that specific antibody level can drop over time. It gets a little technical here but this situation can create the production of antibodies that are associated with new infections. So it can be confusing when a doctor sees new antibody production to Lyme disease but the patient has had symptoms for many years. The doctor thinks that even if the test is accurate, that Lyme disease cannot explain the symptoms a patient has had for many years. This can be one reason patients are told they have a “false positive”.
There are several different lab procedures for testing the presence of antibodies. Two of the most common are the ELISA & the Western Blot tests. Both of these test for antibodies, they just differ in the actual test procedure itself. In North America, conventional medicine has a 2-step process in place to test for Lyme disease (Borrelia only in this case). You must test positive for a certain number of “bands” on an ELISA test (which may be accurate in 35% of cases at best) first before being referred to a Western Blot test. Both are required to be positive for a positive diagnosis. This excludes people who were positive with just one.
It’s important to understand that the Centers for Disease Control (CDC) developed the 2-tiered guidelines (surveillance criteria) for testing to help them track the movement of the infection through the US population. This requires a more stringent testing process than we use clinically when dealing with patients. In this case, the CDC is interested in how the disease is moving across the US, not in whether an individual is positive.
The CDC even states on their website that the surveillance criteria were never designed to be diagnostic criteria (for individual patients), yet conventional medicine has adopted these criteria for diagnosing patients. This means people who don’t mean the stringent criteria for testing positive are being told they do not have Lyme disease when in fact they do.
There are other tests being used now called T-cell activation tests. They differ from antibody testing in that they are attempting to delineate active infections from older infections. These are poised to becoming the preferred method of testing.
Maybe the biggest issue that encompasses all the testing methods is that they do not account for all the possible species of these infections. Lyme disease used to be thought of as an infection with the bug, Borrelia burgdorferi. We now know there are other species of Borrelia including: Borrelia afzelii, Borrelia miyamotoi, Borrelia recurrentis, Borrelia japonica, Borrelia garinii, etc. However, our current tests do not look for all of these species.
Hopefully through the last 2 blog posts, you’ve learned that:
- Lyme disease is an infection with a Borrelia species
- Biting insects like ticks carry more than just Borrelia infections
- Many people have multiple infections, not just Borrelia
- Some of these other infections can make a Borrelia test appear negative
It important to test for all of the infections that are associated with Lyme disease….not just Borrelia.
Contact the Advanced Naturopathic Medicine Centre to obtain tests for all of the infections associated with Lyme disease.
This is one of the more confusing topics related to Lyme disease and I only scratched the surface. It will be covered in more detail in a webinar to follow….
Featured Recipe
Veggie Butternut Squash Pasta
Contributed by Katie

